AI Applications in Medical Diagnosis and Imaging That Are Redefining Healthcare
Explore how AI applications in medical diagnosis and imaging are revolutionizing radiology and pathology to enhance accuracy, speed, and patient care.
Artificial intelligence isn't some far-off concept in healthcare anymore. It’s here, right now, working as a powerful clinical tool that's making a real difference in patient outcomes. Think of AI applications in medical diagnosis and imaging as a highly skilled assistant for clinicians. These sophisticated algorithms analyze medical scans—like X-rays and MRIs—with incredible speed and precision, catching subtle patterns that the human eye might miss.
This technology doesn't replace doctors; it enhances their ability to diagnose diseases earlier and with greater accuracy.
The New Era of AI in Medical Diagnosis
We're stepping into a new reality for healthcare, one where artificial intelligence is fundamentally changing how clinicians work. This isn't just theory—these are practical tools that sharpen human expertise. From spotting tiny anomalies in a radiologist's scan to predicting how a disease might progress, these advancements are elevating the standard of care.
For any healthcare organization looking to get ahead, the first step is simply understanding what’s possible with the AI solutions available today. This guide is your starting point, breaking down the core concepts for leaders ready to make a change. The ultimate goal? Better tools for clinicians, better outcomes for patients, and a more efficient healthcare system for everyone.
A Rapidly Growing Market
The momentum here is impossible to ignore, and the market numbers tell the story. The global AI in diagnostics market has already hit USD 1.94 billion, a clear sign of its deep integration into medical workflows. But that's just the beginning. Projections show it soaring to USD 10.28 billion by 2034, with a compound annual growth rate of 20.37%.
What's driving this explosive growth? It comes down to AI's remarkable precision in analyzing medical images, making sense of electronic health records, and finding patterns that are nearly invisible to us. Radiology is a standout, emerging as the fastest-growing segment. Advanced AI software is now pulling together data from CT scans, MRIs, and even genomics to catch diseases with more certainty. Companies are proudly displaying their work on the world stage, with examples like Orange Neurosciences presenting Canadian digital health innovation at major events.
Core Technologies Driving the Change
Several key AI technologies are powering this diagnostic shift. Each has a specific job, but they all work together to make sense of complex medical data. To clarify their roles, here’s a quick breakdown:
Key AI Technologies Transforming Medical Diagnostics
| AI Technology | Primary Function in Diagnostics | Example Application |
|---|---|---|
| Machine Learning (ML) | Learns from large datasets to predict outcomes without explicit programming. | Predicting a patient's risk for heart disease based on their health records and lab results. |
| Deep Learning | Uses complex neural networks to find intricate patterns, especially in images. | Identifying cancerous nodules on a lung CT scan that might be too small for the naked eye. |
| Computer Vision | Trains computers to "see" and interpret visual information from the real world. | Analyzing pathology slides to count cells or flag abnormal tissue structures for a pathologist. |
These technologies aren't just academic concepts; they are the engines behind a new generation of diagnostic tools.
At the heart of it all are a few core technologies that you’ll hear about often:
- Machine Learning (ML): This is the foundation. ML algorithms learn from massive amounts of data to spot patterns and make predictions. In a clinical setting, an ML model could analyze a patient's health records and predict their risk for developing a specific condition.
- Deep Learning: Think of this as a more advanced, powerful subset of machine learning. It uses layered "neural networks" to analyze data in incredible detail. This is the technology that fuels most modern image recognition, giving AI the ability to interpret scans with near-human levels of understanding.
- Computer Vision: This is the branch of AI that teaches computers to see and understand the visual world. In medicine, this is a game-changer. It allows AI to process and analyze everything from X-rays to pathology slides, automatically flagging areas that need a closer look. Our guide on AI in healthcare dives deeper into these applications.
How AI Is Sharpening the Focus of Medical Imaging
Nowhere is AI’s impact on diagnostics more obvious than in medical imaging. We’re seeing advanced computer vision models interpret incredibly complex scans—X-rays, CTs, MRIs—with a level of detail that often rivals, and sometimes surpasses, the human eye. This is a massive shift for fields like radiology, pathology, and dermatology.
The magic behind these systems is data. They are trained on enormous libraries of medical images, allowing them to learn the subtle visual cues of disease. Think of it as a radiologist who has studied millions of scans instead of thousands. This sheer volume of experience helps the AI spot tiny details, measure disease characteristics, and automatically map out anatomical structures. This, in turn, frees up clinicians to focus their expertise on the most challenging cases.
Making Scans Clearer and Diagnoses More Confident
One of the first things AI does in the imaging pipeline is improve the quality of the scan itself. AI-powered algorithms can clean up "noise" in an MRI or sharpen the details in a low-dose CT scan. It’s a lot like digitally restoring an old photo—critical details that were once fuzzy suddenly pop into focus, giving clinicians a much clearer picture to work with.
This directly translates to more confident diagnoses. When a radiologist can clearly see the edges of a potential tumor, they can make a more precise call, which often means fewer follow-up scans and less need for invasive procedures. It’s a powerful way to elevate the quality of care right from the start.
Real-World Use Cases in Action
AI in imaging isn't just theory; it’s already at work in hospitals and clinics. Exploring these real-world use cases shows just how integrated this technology has become across different medical specialties.
- Radiology: AI tools are busy flagging suspicious nodules in lung CT scans, identifying early signs of stroke in brain MRIs, and spotting hairline fractures in X-rays that might otherwise be missed during a hectic shift.
- Pathology: In the world of digital pathology, AI analyzes high-resolution images of tissue samples. It can count cells, classify cancer subtypes, and even predict how a patient might respond to treatment—tasks that are incredibly tedious and time-consuming for a human.
- Dermatology: AI models, fed with thousands of images of skin lesions, are helping dermatologists differentiate between a harmless mole and a potentially cancerous melanoma with impressive accuracy.
In each scenario, the AI acts as a tireless second set of eyes, making sure that even the smallest anomalies are brought to a specialist’s attention.
Pushing Past Human-Level Accuracy
The performance of these AI systems isn't just on par with human experts; in many cases, it’s better. In cancer diagnostics, AI-powered tools have hit some incredible benchmarks, including a 93% match rate in detecting cancers from imaging analysis.
Consider a study from South Korea where an AI model achieved 90% sensitivity in diagnosing breast cancer from scans, a significant jump from the 78% managed by radiologists. That same model hit 91% accuracy in early detection, while human experts reached 74%. You can dig into the full research about these AI-powered diagnostic findings on scispot.com.
This isn't just about numbers; it highlights AI's ability to process incredibly complex visual data. For radiologists, it provides a reliable co-pilot that quickly flags potential issues, making the entire diagnostic workflow faster and safer for patients.
This kind of precision has a direct impact on patient outcomes. Finding diseases like cancer early and accurately is almost always the key to successful treatment. For organizations looking to get started, an initial AI strategy consulting session is often the best first step to pinpoint where this technology can make the biggest difference.
Using Predictive Diagnostics to Enable Proactive Care
While spotting existing diseases is a huge leap forward, the real frontier for AI applications in medical diagnosis and imaging is in prediction. Instead of just reacting to a patient's current state, AI gives clinicians a powerful tool to look into the future—forecasting disease risk and predicting outcomes long before symptoms ever appear. This is a fundamental shift from reactive to proactive care, and it’s a total game-changer for both individual patients and public health.
How does it work? These predictive models are designed to chew through massive, complex datasets. They sift through everything from electronic health records (EHRs) and genomic data to lab results and imaging scans, hunting for subtle patterns and correlations that signal a future health problem. Think of it as connecting thousands of tiny, seemingly unrelated dots to create a surprisingly clear picture of a patient's health journey.
For example, an algorithm might flag a specific combination of biomarkers, family history, and lifestyle choices that puts someone at an unusually high risk for a heart attack in the next five years. Armed with that knowledge, a doctor can intervene with preventative strategies, potentially turning a future emergency into a non-event.
From Data Points to Life-Saving Predictions
The potential here is enormous and growing every day. In hospitals, AI models are already being used to identify patients at high risk for developing sepsis, a deadly condition, by constantly monitoring real-time data from vital signs and lab work. By flagging at-risk individuals hours before the situation becomes critical, these systems give medical teams a crucial head start.
In the same vein, predictive analytics can forecast which patients are most likely to be readmitted to the hospital after being discharged, allowing care teams to provide targeted follow-up and support. Building these sophisticated models often requires specialized solutions like custom healthcare software development that can securely pull together all these different data sources and plug the algorithms right into the clinical workflow.
And this predictive power isn't confined to the hospital. Beyond imaging, predictive diagnostics can pull actionable insights from a wide array of data, like routine blood tests for comprehensive health checks, to paint an even richer picture of a patient's health profile.
Building Scalable and Clinically Useful Tools
Creating a predictive model is one thing, but turning it into a reliable and scalable clinical tool is a whole other challenge. A successful rollout hinges on a well-thought-out development process that focuses just as much on real-world usability as it does on technical performance. It's about building tools from the ground up to be accurate, scalable, and easy for a clinician to use in their day-to-day routine.
The process usually breaks down like this:
- Data Aggregation and Cleaning: First, you have to gather and standardize huge amounts of patient data from all sorts of different systems.
- Model Training and Validation: Next, you use historical data to train the algorithm and then rigorously test its predictive accuracy against outcomes you already know.
- Clinical Workflow Integration: The tool has to be embedded into existing systems, like the EHR, so that alerts and predictions pop up for clinicians in a way they can actually act on.
- Continuous Monitoring and Refinement: Finally, you have to keep an eye on the model's performance in a live setting and retrain it with new data to keep it sharp and accurate over time.
A predictive model is only as good as the data it’s trained on and its ability to deliver insights when and where they matter most. The goal is to create a seamless feedback loop where data informs prediction, prediction informs action, and the outcomes of that action feed back into the model.
For organizations looking to dip their toes in the water, tools like our Diagnoo platform can help teams validate their AI ideas before committing major resources. You can learn more about how to prototype and test AI diagnostic concepts with Diagnoo. This approach minimizes risk and makes sure you're investing in solutions that have a real shot at making a clinical impact. The future of healthcare isn't just about treating sickness; it's about predicting it, preventing it, and keeping people healthier for longer.
Implementing AI into Clinical Workflows
Bringing AI into a hospital or clinic is a whole lot more than just installing new software. Think of it as a deep integration—weaving these powerful tools right into the fabric of daily clinical work. For any healthcare leader, this means drawing up a practical roadmap that guides the organization from a bright idea to a full-scale rollout, all without disrupting patient care.
The journey kicks off with a detailed look at your specific needs. You have to define exactly what problem the AI will solve and how it will talk to existing systems like your EHR. From there, it's about navigating the maze of data privacy regulations like HIPAA, validating the AI model’s accuracy with your own clinical data, and, most importantly, getting your medical teams ready for a new way of working. Getting these foundational steps right is non-negotiable for a smooth transition, as we explored in our AI adoption guide.
From Pilot To Practice: A Phased Approach
Jumping straight into a hospital-wide deployment is a recipe for chaos. A phased approach is always smarter. It lets you learn and adjust, ensuring the technology is both effective and actually embraced by clinicians. This methodical process minimizes risk and builds the momentum you need for wider adoption.
The first step is always the pilot project. You pick a single, high-impact use case—say, flagging potential strokes on CT scans in the ER—and deploy the AI in a controlled setting. The goal here is simple: measure its real-world performance, gather honest feedback from a small group of users, and iron out any technical wrinkles.
Once the pilot proves its worth, the next move is a limited rollout to a larger department or clinical area. This phase is all about testing how well the system scales and understanding its impact on broader workflows. Only after refining the process and showing clear, undeniable value can you confidently move to a full-scale deployment across all relevant parts of the organization.
Building The Right Support Systems
For any AI tool to really work, it needs a solid support structure behind it. This means creating internal tooling that lets your IT teams monitor the AI's performance, manage updates, and troubleshoot issues without getting in the way of clinical operations. It also means establishing clear protocols for when and how clinicians should act on the insights the AI provides.
For those repetitive but absolutely critical diagnostic tasks, AI Automation as a Service can be a game-changer. This approach can seriously streamline workflows by automatically analyzing routine scans, which frees up your radiologists to focus their expertise on the more complex and ambiguous cases. Essentially, the AI becomes a tireless assistant that handles high-volume work with unshakable accuracy. Understanding the complete AI Product Development Workflow is key to building these systems for long-term success.
Navigating Change And Ensuring Adoption
Technology is only half the battle; the people are the other half. The good news is that the adoption of AI in diagnostics is picking up speed fast. By early 2024, physician usage of AI in this field hit 66%, a staggering 78% increase from the year before. This rapid uptake is largely because of better integration, with around 80% of acute care hospitals now sourcing AI models directly from their EHR vendors.
The diagram below shows how this works in practice, moving from simple data collection to proactive, AI-driven intervention.
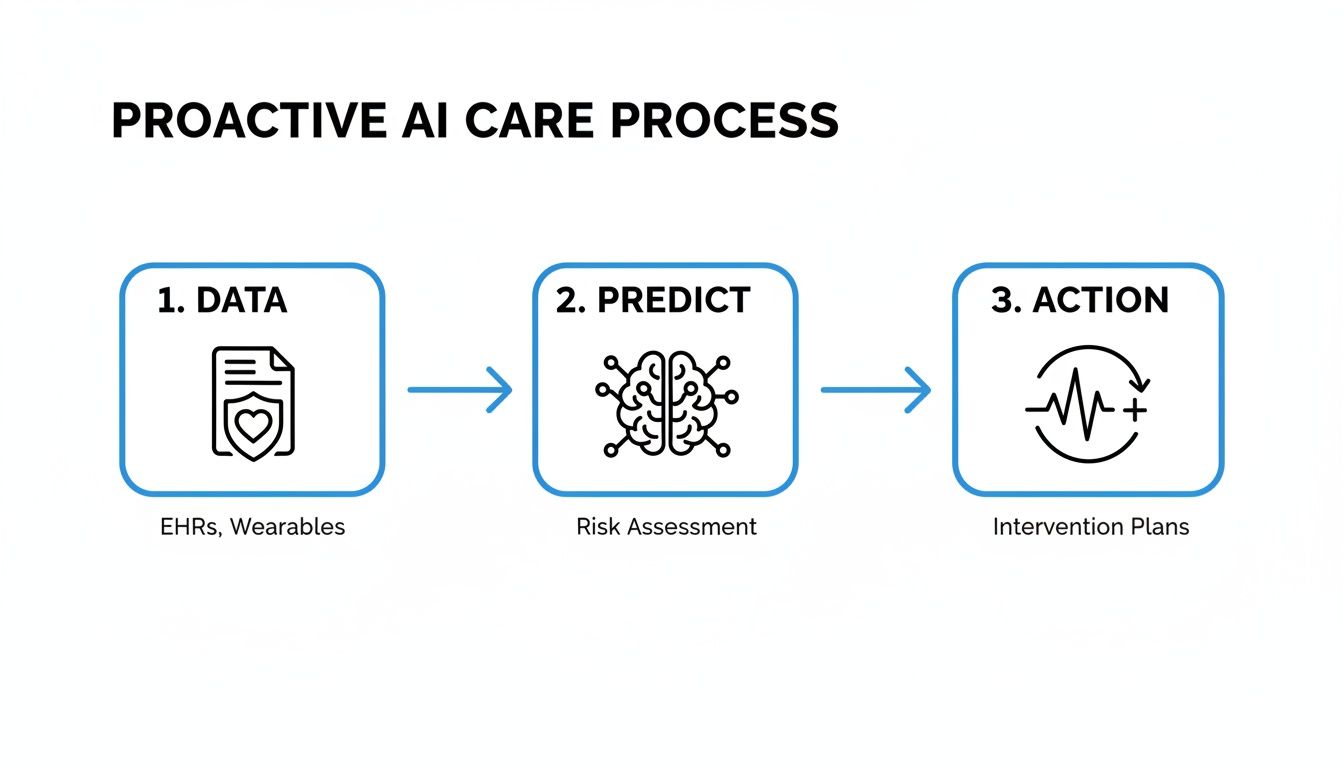
As you can see, it's a clear progression: patient data is analyzed to predict health risks, which then triggers a specific clinical action plan.
To make sure your clinicians actually trust and use these new tools, you have to nail the change management. This means focusing on three key areas:
- Education and Training: Provide hands-on training that shows clinicians exactly how the AI works, what its limitations are, and how it will genuinely make their daily work better.
- Clear Communication: Talk openly about the goals of the AI implementation. Address concerns about job replacement head-on and consistently reinforce the idea of AI as a supportive tool, not a replacement.
- Involving Clinical Champions: Find respected clinicians to champion the new technology. Their job is to share success stories, answer questions, and provide that crucial peer-to-peer support.
A practical implementation roadmap is the best way to structure this journey. The table below outlines the key phases and what to focus on at each step.
AI Implementation Roadmap for Healthcare
| Phase | Key Activities | Primary Consideration | Success Metric |
|---|---|---|---|
| Phase 1: Discovery & Strategy | Identify use cases, define business goals, assess data readiness, form a cross-functional team. | Aligning AI goals with clinical needs and proving a clear ROI. | A well-defined pilot project scope with executive buy-in. |
| Phase 2: Pilot Program | Select vendors, integrate with a test environment, train a small user group, and validate model performance. | Ensuring the AI performs accurately and safely in a controlled, real-world setting. | Pilot meets or exceeds predefined accuracy and efficiency benchmarks. |
| Phase 3: Limited Rollout | Expand to a full department, refine workflows based on feedback, monitor system scalability. | Managing the impact on departmental operations and clinician workflows. | Positive user feedback and demonstrated improvements in departmental KPIs. |
| Phase 4: Full-Scale Deployment | Deploy across all relevant settings, establish ongoing governance, and create a long-term monitoring plan. | Ensuring robust technical support and a continuous feedback loop for improvements. | Widespread adoption, sustained ROI, and measurable impact on patient outcomes. |
Following a structured plan like this turns a complex technical challenge into a manageable, step-by-step process focused on clinical value.
Ultimately, a successful AI implementation isn't just a technical project—it's a clinical transformation initiative. It requires a true partnership between IT, clinical leadership, and the frontline staff to ensure the technology empowers clinicians and, most importantly, improves patient outcomes.
Making the Financial Case for AI in Diagnostics
While the clinical breakthroughs are exciting, any new technology has to make sense on the balance sheet. For hospital administrators and practice leaders, that means building a rock-solid business case for AI in medical diagnosis and imaging. We have to look past the impressive tech specs and figure out the real, measurable return on investment (ROI).
The financial upside isn't always obvious at first glance, but it's significant. The benefits really fall into two buckets: direct savings from making your operations run smoother and indirect value from improving patient health. When you add them up, they make a compelling argument for bringing AI into the fold. It stops being a futuristic "nice-to-have" and becomes a smart financial move.
Pinpointing the Direct and Indirect Financial Gains
The easiest place to see the ROI is in direct operational improvements. AI is a workhorse for repetitive tasks, and that saves time and money. Think about the daily diagnostic grind: an AI can pre-screen hundreds of images, flag the ones that need immediate attention, and let radiologists spend their brainpower on the truly complex cases.
This simple change creates a positive ripple effect throughout the entire department:
- Faster Report Turnaround: An AI can read a chest X-ray in a few seconds. That’s a massive reduction in the time it takes to get from scan to diagnosis, helping radiology groups easily hit—and even beat—their service-level agreements.
- Boosted Operational Efficiency: When you automate tasks like measuring a tumor or segmenting an organ, you give your clinical team back their most valuable resource: time. This lets a department absorb a higher volume of scans without having to hire more staff.
- Fewer Diagnostic Errors: AI acts as a tireless second pair of eyes. It can catch subtle anomalies a human might miss at the end of a long shift. Cutting down on errors means fewer costly follow-up scans and a lower risk of malpractice lawsuits.
But the savings don't stop there. The indirect benefits are just as powerful. Better, faster diagnoses naturally lead to better patient outcomes, which have their own financial logic. For example, catching a stroke earlier means quicker treatment, which often translates to shorter hospital stays and less need for long-term, expensive rehabilitation.
This isn't just a technology upgrade; it's about re-engineering the entire system of care. The gains in efficiency and patient health create a financial flywheel that benefits everyone—the hospital, the clinicians, and the patients.
A Framework for Nailing Down the ROI
To make your case to the finance department, you need a clear way to project these gains. It usually starts with a hard look at your current workflow. A Custom AI Strategy report is a great tool for this, as it helps you put real numbers to potential improvements and ensures your AI goals line up with what the organization is trying to achieve.
Your ROI calculation needs to include a few key numbers:
- Productivity Gains: Figure out how much time is saved per radiologist, per day. Then, turn that into a dollar amount based on their salary and how many more cases they can now handle.
- Error Reduction Savings: Estimate what a single diagnostic error costs you—think extra tests, longer hospital stays, and potential legal fees. Then, project the savings you’d see by improving accuracy with AI.
- Shorter Patient Stays: For certain conditions, analyze how a faster diagnosis could get a patient home sooner. Calculate the cost savings for every day you shave off the average length of stay.
It’s Not Just About Saving Money—It’s About Making It
The business case for AI isn't just defensive; it’s also about growth. It can unlock entirely new ways to generate revenue. By offering sophisticated services that rely on AI—like detailed quantitative imaging analysis or predictive risk scores for certain diseases—a hospital or clinic can stand out from the competition.
These premium services can become new billable offerings and attract more patients. Plus, by being one of the first in your area to adopt proven AI tools for business, you build a reputation as an innovator. That kind of leadership helps attract the best clinical talent. In the end, a smart AI investment pays for itself from all sides: cutting costs, boosting efficiency, and creating new opportunities for growth.
Looking Ahead: What's Next for AI in Medical Diagnosis?
The world of AI in medical diagnosis and imaging isn’t standing still. We're on the cusp of some truly exciting developments that go far beyond just refining the algorithms we use today. The next few years will see a shift toward AI that can see the whole picture of a patient’s health, all while grappling with the critical ethical questions that come with such powerful technology.
One of the most significant leaps forward is what we call multimodal AI. Imagine an AI that doesn't just look at a CT scan in isolation. Instead, it reads the scan, the radiologist's written report, the patient's genetic markers, and their entire electronic health record, all at the same time. By pulling these disparate threads together, these systems can spot subtle, interconnected patterns that no single piece of data could ever reveal. This leads to a much deeper, more accurate diagnostic insight.
The Next Wave of AI Innovation
Right alongside this, we have federated learning, a brilliant solution to one of the biggest roadblocks in healthcare AI: data privacy. The traditional approach would be to gather massive amounts of patient data in one central server to train a model—a privacy nightmare.
Federated learning flips that model on its head. The AI model is trained locally, right inside the hospital's own secure system. Only the anonymous mathematical learnings—not the actual patient data—are sent back to a central model to make it smarter. This allows us to build incredibly powerful, large-scale AI from diverse datasets without ever having to move or expose sensitive patient information.
These aren't just minor upgrades. We're talking about a fundamental jump toward AI that understands patient health in a much more holistic way, all while hardwiring privacy into its very design.
Confronting the Ethical Tightrope
As these tools become more embedded in day-to-day care, we have to walk an ethical tightrope. The aim is to push the boundaries of what's possible, but to do so responsibly, ensuring AI serves every patient safely and fairly. For any organization venturing into this space, a solid AI Strategy consulting tool is invaluable for striking that balance between innovation and ethics.
There are a few big challenges that need our constant attention:
- Algorithmic Bias: An AI is a reflection of its training data. If that data is skewed toward one demographic, the tool will inevitably be less accurate for others. This is a huge risk, as it could easily widen existing health disparities if not actively managed.
- Data Privacy and Security: Patient confidentiality is sacred. As we connect more systems, we must build Fort Knox-level security to guard against data breaches and ensure patient information is never misused.
- The Regulatory Gauntlet: Getting a green light from bodies like the FDA is a long and demanding journey for a reason. You have to prove, with hard clinical data, that your AI is not only effective but, more importantly, safe for patient use.
- Keeping the "Care" in Healthcare: We can't forget that medicine is a fundamentally human endeavor. AI should be a co-pilot that enhances a doctor's expertise and frees them up to connect with patients, not a black box that replaces their clinical judgment or the need for empathy.
Tackling these issues isn't easy; it takes a partner who has been there before. Our expert team works with healthcare leaders to build AI systems that are not only effective but also trustworthy, transparent, and built on a strong ethical foundation.
Diving Deeper: Your Questions Answered
Let's tackle some of the most common questions that come up when people start thinking about bringing AI into the world of medical diagnosis and imaging. These are the practical, real-world concerns we hear from healthcare leaders, doctors, and even curious patients.
So, Is AI Going to Replace Radiologists?
That's the big question on everyone's mind, isn't it? The short answer is a resounding no. Think of AI less as a replacement and more as the most sophisticated co-pilot a radiologist could ever ask for.
AI is brilliant at the heavy lifting—sifting through thousands of images to spot subtle patterns that might signal a problem. This frees up the human expert, the radiologist, to focus their invaluable experience on the toughest cases, collaborate with other physicians, and make the final, critical diagnostic call. The future isn't about AI or doctors; it's about AI and doctors working together.
What Are the Toughest Hurdles to Clear When Implementing AI?
Getting AI up and running in a hospital setting isn't as simple as installing new software. The biggest roadblocks usually fall into three camps: data, regulations, and people.
-
The Data Dilemma: AI models are hungry for high-quality, standardized data. But in most hospitals, patient information is spread across different, often incompatible, electronic health record (EHR) systems. Getting all that data into a clean, usable format is a massive challenge.
-
The Regulatory Maze: You can't just plug in a medical AI and go. These tools have to navigate a complex web of rules, from HIPAA for patient privacy to getting formal clearance from the FDA. It's a meticulous and time-consuming process.
-
The Workflow Puzzle: Perhaps the trickiest part is fitting AI smoothly into the way clinicians already work. It requires thoughtful planning, extensive training, and a real commitment to managing change so that the new tool actually helps, rather than hinders, patient care. Nailing the initial AI requirements analysis is absolutely key to getting this right from day one.
How Do We Even Get Started with AI?
It's easy to get overwhelmed, but the best approach is to start small and be strategic. The first step isn't about technology; it's about identifying a genuine problem.
Pick one specific, high-value challenge you're facing. Maybe it's the long wait times for interpreting a certain kind of scan or a high rate of inconclusive initial findings. Focus your efforts there.
Launch a pilot project to test the waters. This lets you see the AI in action, measure its real-world impact, and learn valuable lessons without turning the whole hospital upside down. Partnering with seasoned experts through AI strategy consulting can provide a clear roadmap, help you choose the right tools, and make sure your first foray into AI delivers real, measurable results.
Ready to see what AI can do for your diagnostic and imaging workflows? Ekipa AI can build a custom strategy and implementation plan that turns your biggest challenges into new opportunities for excellence. Our expert team has the experience to guide you every step of the way. Start your AI journey with us today.



