AI-Powered Early Disease Detection Solutions A Practical Guide
Discover how AI-powered early disease detection solutions are transforming healthcare. This guide explores the technology, benefits, and implementation roadmap.
Instead of just treating diseases once they show up, AI-powered early detection systems are flipping the script. They dig through mountains of medical data to find diseases long before a person ever feels sick, moving healthcare from a "wait and see" approach to a proactive, preventative one.
These systems use sophisticated machine learning and deep learning algorithms to spot tiny, almost invisible patterns in everything from medical images and genetic markers to everyday health records—clues that a human might easily miss. This allows for intervention at the earliest possible moment, which can make a world of difference for patient outcomes.
Shifting Healthcare from Reactive to Proactive with AI
Think about a patient, Sarah. She feels completely fine, but deep inside her body, a small group of cells has started to change, marking the very beginning of an aggressive cancer. In our current system, Sarah likely wouldn't notice any symptoms for months, maybe even years. By the time she finally goes to the doctor, the disease could be advanced, making treatment tougher, more expensive, and less likely to work.
This is the fundamental problem with reactive medicine: it waits for the fire alarm to go off instead of looking for the smoke.
This waiting game comes with a steep price, both in human lives and dollars. Late-stage diagnoses almost always mean a worse prognosis, more grueling treatments, and astronomical healthcare bills. The emotional strain on patients and families is impossible to quantify. The system is built to react to crises, not to stop them from happening in the first place.
The Proactive Power of Prediction
This is where artificial intelligence changes the game entirely. Instead of waiting for symptoms to appear, AI-powered early disease detection solutions act like a 24/7 lookout, constantly scanning for the faintest signs of trouble. These systems are trained on millions of data points, from mammograms and CT scans to genomic sequences and electronic health records. By sifting through this ocean of information, AI learns to recognize the subtle signatures that often precede a formal diagnosis.
AI doesn't replace clinicians; it equips them with a powerful new sense. It’s like giving a radiologist a magnifying glass that can see years into the future, highlighting risks before they become realities and enabling a new standard of preventative care.
This capability fundamentally moves the practice of medicine upstream. It allows healthcare organizations to shift from simply managing sickness to actively promoting wellness. A closer look at the different applications of AI in the healthcare industry shows a clear roadmap to more effective and personalized patient care.
Key Benefits of an AI-Driven Approach
Making the switch to proactive detection offers real, measurable benefits for everyone involved. It's not just about finding diseases sooner; it’s about building a smarter, more resilient healthcare system.
- Improved Patient Outcomes: Finding a cancer at Stage 1 instead of Stage 4 can be the difference between a full recovery and a long, difficult fight. Survival rates skyrocket.
- Reduced Healthcare Costs: It’s far cheaper to treat a condition in its infancy than to manage an advanced disease and all its complications. This eases the financial strain on patients, insurers, and hospitals.
- Enhanced Clinical Efficiency: AI can take on the tedious work of analyzing routine screenings, which frees up highly skilled specialists like radiologists and pathologists to focus on the most challenging cases.
- Personalized Prevention Plans: By identifying high-risk individuals, doctors can create customized screening schedules and preventative plans, moving away from generic, one-size-fits-all advice.
By adopting these advanced AI solutions, healthcare leaders can start crafting a future where a late-stage diagnosis is a rare event, not an everyday tragedy.
How AI Uncovers Hidden Patterns in Medical Data
At its heart, AI in medicine works like a super-powered detective. It can spot connections and clues in medical data that are often invisible to the human eye. The system pores over immense volumes of information—from complex MRI scans and genomic sequences to decades of electronic health records—searching for the subtle signatures of disease long before they become obvious. This isn't magic; it's just the smart application of powerful computational techniques.
Think of traditional machine learning as a detective-in-training. You feed it millions of "case files"—for example, labeled medical images of both healthy and diseased tissue. Over time, the algorithm learns to pick out the tell-tale signs of a specific condition. It becomes an expert at spotting that one particular clue, over and over again.

Deep learning takes this a giant leap further. Imagine a radiologist with a perfect, photographic memory of every single scan they've ever seen. Deep learning models, especially neural networks, analyze medical images layer by layer. They don't just identify one pattern but instead see complex combinations of features—subtle textures, shapes, and densities—that correlate with disease, sometimes years before a person ever feels a symptom.
The Fuel for AI: High-Quality Medical Data
These advanced AI-powered early disease detection solutions are completely reliant on the quality and diversity of the data they learn from. Without rich, comprehensive datasets, even the most sophisticated algorithm is useless.
The most critical data types include:
- Medical Imaging: This covers everything from X-rays and CT scans to MRIs and ultrasounds. AI is exceptionally good at analyzing these visual inputs to detect anomalies like tumors, fractures, or early signs of tissue damage.
- Genomic and Proteomic Data: By analyzing genetic sequences and protein structures, AI can pinpoint inherited risk factors and the specific molecular fingerprints of diseases like cancer.
- Electronic Health Records (EHRs): This is a goldmine of unstructured data, including physician notes, lab results, and patient histories. It provides a rich, long-term view of a patient's health, helping AI predict future risks with greater accuracy.
A model trained only on data from one demographic will almost certainly perform poorly on others. Building robust, unbiased AI requires diverse datasets that reflect the entire patient population. This is the only way to ensure equitable and accurate diagnostics for everyone.
This data-first approach is already making a real difference. In many clinical settings, AI systems are now reaching a level of diagnostic performance that rivals, or in some cases even exceeds, human experts. For instance, studies have shown AI models reaching up to 94% accuracy in detecting tumors from scans. In breast cancer screening, some AI models have demonstrated higher sensitivity than human radiologists. These are not just numbers; they translate directly into earlier diagnoses, which can dramatically improve survival rates for diseases where every day counts.
Augmenting Clinicians, Not Replacing Them
It's important to be clear: the goal of these AI solutions is not to replace skilled clinicians. It’s to augment their abilities. AI can take on the time-consuming and repetitive work of screening thousands of images or records, acting as a tireless assistant.
This frees up doctors, radiologists, and pathologists to focus their expertise where it's needed most: on complex cases, patient consultations, and designing treatment plans.
This collaboration creates a powerful synergy. The AI flags potential issues with incredible speed and accuracy, and the human expert provides the critical context, clinical judgment, and empathy that are essential for exceptional patient care. Ultimately, this partnership between human and machine intelligence is what will drive the future of proactive, preventative medicine.
Using Predictive Analytics for Population Health
While AI is making waves in diagnosing individual patients, its true power might lie in protecting the health of entire communities. AI-powered early disease detection solutions are helping us move away from broad, one-size-fits-all public health campaigns and toward something much more precise and data-driven. This approach leans heavily on predictive analytics to spot groups at high risk for chronic conditions long before anyone shows symptoms.
Think about it: what if you could forecast a flu outbreak in a specific zip code or pinpoint a community where the risk of type 2 diabetes is quietly climbing? By sifting through huge, anonymized datasets—things like demographics, local environmental factors, and public health records—AI models can spot these large-scale trends. This allows healthcare systems to stop being purely reactive and start deploying targeted, preventive strategies right where they’ll do the most good.
Successfully rolling out these models isn’t just about the tech; it requires thoughtful planning to manage data ethically and effectively at scale. If you're looking to get a better handle on the core techniques that make this kind of proactive healthcare possible, it’s worth digging into resources like a guide to predictive analysis machine learning.
From Broad Strokes to Targeted Interventions
For a long time, public health has relied on generalized campaigns, like posters in every pharmacy encouraging flu shots. These efforts are well-intentioned, of course, but they often lack focus and miss the people who need the message most. Predictive analytics allows for a far more surgical approach.
Instead of a generic message blasted out to everyone, a health system could:
- Send personalized reminders for colon cancer screenings directly to individuals whose genetic or lifestyle data flags them as high-risk.
- Launch localized diabetes prevention programs right in the neighborhoods where data shows a spike in prediabetic markers.
- Proactively dispatch mobile clinics and other resources to specific areas showing the very first warning signs of a potential viral outbreak.
This isn’t just about efficiency; it’s about impact. This level of precision ensures that precious resources reach the right people at the right time. It’s a fundamental shift from public health broadcasting to public health narrowcasting.
The Power of Scale in Predictive Health
The real-world results of this approach are proving to be incredibly powerful, especially at scale. AI-driven analytics are flagging at-risk individuals before they even feel sick, opening the door for interventions that dramatically cut down on future costs and suffering.
For example, one study used a machine-learning model to analyze the health records of roughly 500,000 UK participants. The model was able to predict the onset of over 1,000 different diseases, sometimes years before a doctor would have made a clinical diagnosis. This proves that we can predict multiple diseases at once across a massive population.
By identifying risks at the population level, healthcare organizations can intervene before a health issue becomes a crisis. This not only improves patient outcomes and reduces health disparities but also creates a more financially sustainable healthcare ecosystem by preventing chronic diseases from taking hold in the first place.
This strategic pivot—from treating sick individuals to preventing entire communities from getting sick—is a cornerstone of modern medicine. It's about getting ahead of the problem. As the data consistently shows, prevention is almost always more effective and far more economical than treating a disease in its advanced stages.
The Business Case for Investing in AI Diagnostics
Bringing AI-powered early disease detection into your practice isn't just a clinical upgrade—it's a smart business move with a very real, very compelling return on investment (ROI). For healthcare leaders, the financial argument is just as powerful as the clinical one. It’s a case built on making your operations leaner, cutting long-term costs, and gaining a serious competitive edge. The conversation has moved past "if" we should adopt this technology; now, it's about "how fast" we can, because the financial proof is right there in the numbers.
This isn't some far-off future idea, either. It’s happening now. The U.S. market for AI diagnostics is already valued at around $790 million, and a flood of global investment is pushing it forward. What’s fueling this? Tangible results. We’re seeing AI tools that can slash diagnostic turnaround times from days down to minutes, which directly cuts the cost of each screening compared to relying solely on traditional specialists. If you want to dig deeper into these trends, you can discover more insights on the commercialization of AI in healthcare.
Driving Operational Efficiency and Throughput
Right out of the gate, one of the biggest financial wins comes from smoothing out your diagnostic workflows. AI algorithms can churn through medical images or lab results at an incredible pace, handling the routine screenings automatically and flagging the high-priority cases that need a human expert's eyes right away. This directly impacts your bottom line.
- Faster Turnaround: When analysis is quicker, diagnoses come faster. This lets physicians start treatment sooner and, just as importantly, see more patients.
- Lower Screening Costs: AI takes on the high-volume, repetitive work, meaning less manual effort is needed for every single screening. That’s a direct cut to your operational expenses.
- More Patients, Same Footprint: With more efficient processes, your facility can handle a greater volume of patients without needing to build new wings or hire more staff.
These aren't just abstract benefits. A lot of organizations are already turning to AI Automation as a Service to fine-tune their diagnostic pipelines, effectively converting operational speed into a significant financial plus.
The Long-Term Financial Impact of Early Detection
Beyond the immediate savings, the real game-changer is how early detection slashes long-term costs. It’s simple, really: treating a disease in its earliest stages is almost always less invasive, less complicated, and dramatically cheaper than managing a crisis down the road.
Think of investing in early detection as a strategic play to lower the total cost of care over a patient's entire life. By catching diseases sooner, you sidestep the multi-million dollar price tags that come with late-stage cancer treatments, chronic disease management, and emergency interventions.
Presenting these advantages with real-world use cases offers concrete evidence that powerful AI tools for business are a direct investment in an organization's financial health. It's about being proactive and preventing the most expensive health crises before they even start.
Of course, building a solid financial model means you need to truly understand what your organization needs. This is where an initial AI requirements analysis becomes invaluable. A partnership with our expert team can help you map out the potential ROI and craft a business case that makes sense for both your clinical goals and your financial ones.
A Strategic Roadmap to AI Implementation
Jumping into AI-powered diagnostics isn't about buying a piece of software; it's about making a fundamental shift in clinical operations. To make this leap successfully, healthcare leaders need a clear, methodical plan. This journey doesn’t start with technology—it starts with strategy.
The first, and frankly most important, step is laying a solid foundation. This is where a detailed implementation support plan proves its worth. It forces you to take an honest look at your organization's specific needs, clinical goals, and current infrastructure. This ensures any AI initiative you launch is genuinely aligned with your long-term vision, not just a tech-for-tech's-sake project.
Foundational Steps for Successful Adoption
With a clear strategy in hand, the real work begins. This phase is all about carefully sizing up what you have internally and what the outside world—especially regulators—demands.
- Assess Data Readiness: An AI model is a reflection of the data it learns from. You have to evaluate the quality, volume, and diversity of your existing data, whether it's buried in EHRs or stored in medical imaging archives. This step almost always uncovers data gaps and highlights the need for better data governance.
- Navigate the Regulatory Landscape: Healthcare is, for good reason, a minefield of regulations. Any AI tool you deploy must be rock-solid compliant with standards like HIPAA in the United States or GDPR in Europe. Getting a handle on these requirements from day one is non-negotiable and saves a world of headaches later.
- Address Ethical Considerations: You have to tackle thorny issues like model bias head-on. This means ensuring any AI you consider was trained on datasets that truly reflect your patient population. Otherwise, you risk worsening health disparities. Transparency is also crucial; clinicians and patients need to understand, at a high level, how the AI is making its recommendations to build trust.
Getting these foundational pieces right sets the stage for a smooth deployment, making sure your organization is prepared technically, legally, and ethically for the road ahead.
This flow chart shows how a well-executed AI diagnostics program creates a positive feedback loop, driving value from faster workflows all the way to better patient health.
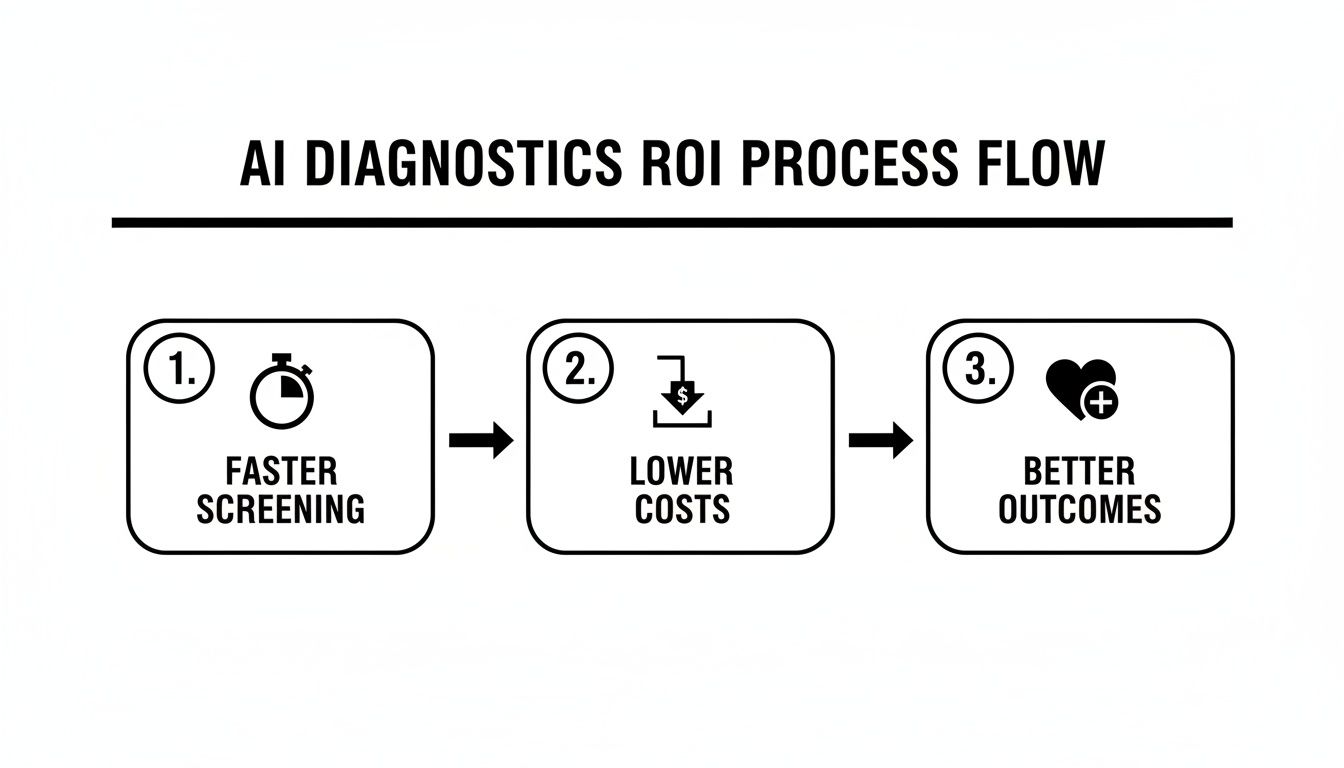
As the visual makes clear, the value chain starts with immediate gains in screening efficiency, which leads directly to lower operational costs and, most importantly, to much better long-term outcomes for patients.
Choosing Partners and Managing Change
With a strong foundation in place, your focus can shift to picking the right tools and, just as importantly, preparing your team for the change. This is all about finding a partner who can weave new technology into your existing clinical workflows without causing chaos.
A critical part of this is choosing the right technology vendors. It’s about much more than just an algorithm's accuracy score. You have to be certain the solution can integrate cleanly with your current EHR and IT systems.
The human side of this transition is every bit as critical as the technology. A thoughtful change management strategy is the only way to get clinical staff on board and build their confidence in these new tools.
This means providing thorough training, communicating clearly about how the AI helps them do their jobs better, and constantly reinforcing that it's a tool to augment their expertise—not replace it. Fostering a culture where clinicians and technology work together is one of the biggest predictors of success.
By following a structured roadmap that moves from initial strategy to pilot programs and eventually to a full-scale rollout, healthcare organizations can navigate the complexities of AI adoption with confidence. This deliberate planning makes the transition smoother, ensures your investment pays off, and helps the technology achieve its ultimate goal: improving and saving lives.
Vendor Evaluation Framework for AI Detection Solutions
Choosing the right technology partner is one of the most critical decisions in your AI implementation journey. This framework provides a checklist of key criteria to help you vet potential vendors and ensure you find a partner that aligns with your clinical, technical, and business needs.
| Evaluation Criteria | Key Questions to Ask | Importance (High/Medium/Low) |
|---|---|---|
| Clinical Validation & Accuracy | Has the algorithm been validated in peer-reviewed studies? What is its documented accuracy, sensitivity, and specificity for our patient demographic? Is it FDA-cleared or CE-marked? | High |
| Data Requirements & Security | What specific data (type, format, volume) does the model require? How is data protected both in transit and at rest? Does the vendor comply with HIPAA/GDPR? | High |
| Integration & Workflow | How does the solution integrate with our existing EHR, PACS, and other IT systems? Is the user interface intuitive for clinicians? Can it be customized to fit our workflow? | High |
| Model Transparency & Bias | Can the vendor explain how the model arrives at its conclusions (explainability)? On what demographic data was the model trained? What steps were taken to mitigate bias? | High |
| Scalability & Performance | Can the solution handle our current and future patient volume? What is the average processing time per case? What are the hardware and infrastructure requirements? | Medium |
| Vendor Support & Training | What level of technical support is provided during and after implementation? What training programs are available for our clinical and IT staff? | Medium |
| Total Cost of Ownership (TCO) | What is the pricing model (e.g., subscription, per-scan)? Are there additional costs for integration, maintenance, or upgrades? What is the expected ROI? | Medium |
| Regulatory & Compliance | Does the vendor have a clear roadmap for future regulatory updates and submissions? How do they handle post-market surveillance and model updates? | Low |
Using a structured framework like this helps turn a potentially overwhelming decision into a manageable process. It ensures you’re asking the right questions and prioritizing the factors that will have the biggest impact on a successful, long-term partnership.
Partnering for a Future of Proactive Medicine
The road to AI-driven healthcare isn't a solo journey. Realizing the full potential of AI-powered early disease detection happens when healthcare innovators and technology experts build a true partnership. Success is all about bridging the gap between a complex algorithm and its practical, day-to-day use in a clinic—making sure the tech always serves the patient first.
There’s no doubt about it: the future of medicine is predictive, personalized, and proactive. Getting on board with these new capabilities is a must for any healthcare organization that wants to lead the pack in patient care. This shift isn't just about installing new software; it's about having a strategic vision for what's possible.
Forging the Right Technical Partnership
Going from a promising idea to a clinical reality requires a partner who brings more than just code to the table. They need to have deep domain expertise and a genuine feel for the healthcare landscape. This is where offerings like AI Automation as a Service really make a difference, helping you weave advanced systems into your existing workflows without causing chaos.
A great technology partner should help you:
- Develop custom AI solutions that solve the specific clinical challenges you actually face. This can include anything from diagnostic tools to custom healthcare software development.
- Build smart internal tooling that makes your staff's lives easier, not harder.
- Follow a proven AI Product Development Workflow that keeps projects on track and focused on delivering real results.
The most successful AI implementations are born from collaboration. They combine the clinical wisdom of healthcare professionals with the technical skill of AI specialists to create tools that are both powerful and practical.
This kind of hands-on, collaborative approach is the only way to ensure the final product isn't just a cool piece of tech, but something genuinely useful in a busy, real-world clinical setting.
Take the Next Step Toward Proactive Care
Bringing AI into your organization is a strategic move that fundamentally changes how you deliver healthcare. It gives clinicians powerful new tools, improves patient outcomes, and ultimately builds a more resilient, efficient system for everyone. That journey starts with a clear plan and the right people to guide you.
We encourage healthcare leaders to take that next step. Connect with our expert team to explore how a tailored AI strategy, backed by a deep understanding of both technology and medicine, can completely reshape your approach to patient care.
Frequently Asked Questions
What diseases can AI help detect early?
AI's diagnostic reach is broad and continually expanding. Key areas include:
- Oncology: Identifying potential tumors in mammograms, CT scans, and other medical images, often detecting subtle patterns missed by the human eye.
- Cardiology: Analyzing electrocardiograms (ECGs) to spot faint signals of arrhythmia or other cardiac risks that might otherwise go unnoticed.
- Neurology: Detecting early signs of neurodegenerative diseases, such as Alzheimer's, by analyzing changes in brain scans long before major symptoms appear.
- Diabetic Retinopathy: Screening retinal images for early signs of eye disease in diabetic patients, a leading cause of blindness.
How critical are data quality and privacy?
They are absolutely fundamental. An AI model's accuracy is directly dependent on the quality of the data it's trained on. Using biased, incomplete, or low-quality data will lead to unreliable and unfair outcomes. Furthermore, protecting patient privacy is non-negotiable. Any AI solution used in a clinical setting must be fully compliant with regulations like HIPAA to maintain the trust of both clinicians and patients.
How can a hospital realistically get started with AI?
Adopting AI doesn't require a complete overhaul of your systems overnight. The most successful approach is to start with a focused pilot project.
- Identify a High-Impact Use Case: Choose a specific area, like radiology or pathology, where AI can solve a clear problem.
- Conduct a Needs Analysis: Work with an AI specialist to define goals, assess data readiness, and create a clear roadmap.
- Launch a Pilot: Implement the solution on a small scale to test its effectiveness, gather feedback from staff, and demonstrate ROI.
- Scale Strategically: Use the insights from the pilot to inform a wider, phased rollout across the organization.
This step-by-step method, often guided by expert AI strategy consulting, minimizes risk and builds momentum for a successful transformation.
Will AI replace radiologists and other clinicians?
No, the goal of AI in healthcare is augmentation, not replacement. AI tools act as powerful assistants, handling repetitive, high-volume tasks like screening thousands of images. This frees up highly skilled clinicians to focus on complex cases, patient consultations, and treatment planning, where their expertise and empathy are irreplaceable. It creates a collaborative synergy between human intelligence and machine efficiency.
Ready to build a more proactive, data-driven future for your healthcare organization? Ekipa AI delivers tailored AI strategies that turn complex opportunities into scalable, real-world impact. Start your AI transformation journey today.



