Explore the Use of Machine Learning in Radiology and Pathology: Practical Guide
Discover the use of machine learning in radiology and pathology and how AI is driving real-world diagnostics, workflows, and future trends.
The practical use of machine learning in radiology and pathology is rapidly shifting from a futuristic idea to a clinical reality. It’s helping medical teams get a handle on ever-growing workloads and the sheer complexity of modern diagnostics. These smart algorithms are trained to analyze medical images—think CT scans or digital pathology slides—and spot subtle patterns that might otherwise be missed, boosting both the speed and accuracy of a diagnosis.
The New Diagnostic Frontier: How ML Is Reshaping Medical Imaging
The pressure on radiologists and pathologists has never been higher. They face a relentless flood of complex cases, pushing many toward burnout and creating diagnostic backlogs that affect patient care. This isn’t just a problem; it’s an inflection point, opening the door for a much-needed change in how we work.
Machine learning is stepping in to offer a path forward. It acts as a powerful co-pilot, designed to enhance the skills of medical experts and bring a new level of precision and efficiency to the diagnostic workflow.
Augmenting Human Expertise
Let's be clear: ML in medical imaging isn’t about replacing specialists. It’s about collaboration. Picture an ML model as an incredibly thorough assistant that can pre-screen thousands of images, flagging suspicious areas for a human expert to review.
This partnership lets clinicians zero in on the most challenging parts of a case, applying their deep experience where it counts the most. The benefits are tangible and immediate:
-
Increased Speed: An ML algorithm can sift through massive image datasets in a fraction of the time it would take a person, which means faster report turnarounds for patients.
-
Enhanced Accuracy: By identifying patterns too subtle for the human eye, these tools can help lower the rate of false negatives and give clinicians more confidence in their findings.
-
Workflow Optimization: Automating routine, repetitive tasks frees up specialists from tedious work, letting them manage a higher caseload without sacrificing quality.
A Roadmap for Transformation
Throughout this guide, we’ll dig into the real-world applications of machine learning in diagnostics. We’ll move past the hype to look at specific clinical use cases, from classifying tumors to predicting how a disease might progress. We will also lay out a practical roadmap for getting started, showing how powerful AI solutions are becoming essential tools for modern healthcare.
The real goal here is to pull back the curtain on the technology and give you a clear-eyed view of how it fits into today's clinical environments. Getting from strategy to deployment is a structured journey, not a leap of faith.
For example, our PathWise AI model is already showing how specialized tools can give pathologists critical support in their daily work. By understanding these on-the-ground applications, healthcare organizations can start to map out their own journey toward a more efficient and accurate diagnostic future.
What Machine Learning Actually Does in Diagnostics
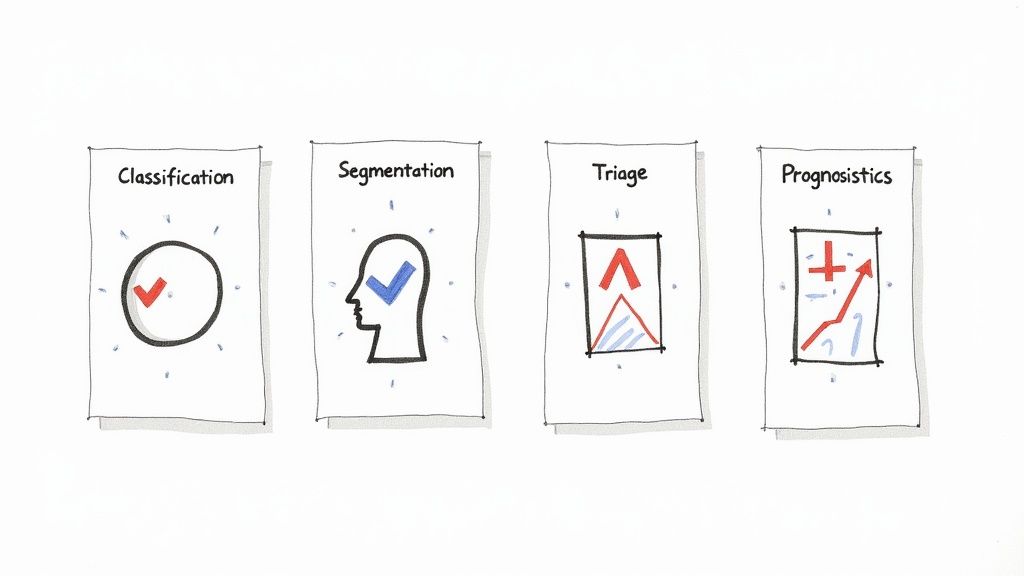
To really grasp how machine learning is used in radiology and pathology, you have to look beyond the hype and see what these algorithms are actually doing. It’s less like a single magic wand and more like a highly specialized toolkit, with each tool designed for a specific, critical job.
These core functions are the fundamental building blocks that empower AI to help clinicians make faster, more confident decisions. They handle the heavy lifting of complex analysis, turning enormous amounts of visual data into clear insights that can directly improve patient care and make the entire diagnostic workflow more efficient.
Classification: Sorting the Ambiguous from the Normal
At its most basic level, classification is about sorting things into buckets. In diagnostics, this translates to answering a simple but profound question: "Is this finding suspicious or not?" An ML model, after being trained on thousands of labeled images, learns to recognize the incredibly subtle patterns—texture, density, shape—that separate a malignant finding from a benign one.
A classic example comes from dermatology, where an algorithm can look at a photo of a skin lesion and classify it as likely melanoma or just a harmless mole. This provides a quick preliminary assessment, helping doctors prioritize who needs a biopsy right away.
This ability to provide a clear, binary answer is a cornerstone of many AI tools for business because it cuts through complexity. The same principle is just as powerful in a chest X-ray or a digital pathology slide, offering a first-pass analysis that guides the next steps.
Segmentation: Drawing the Lines with Precision
While classification answers "what is it?", segmentation answers "where is it?". This task is all about meticulously drawing a boundary around a specific region of interest in an image. For an oncologist, that could mean perfectly outlining a tumor on a CT scan or a cluster of cancerous cells on a digital slide.
Picture a radiation oncologist mapping out a treatment plan for a brain tumor. A segmentation model can automatically delineate the exact contours of the tumor and, just as importantly, the critical healthy structures right next to it, like the optic nerve.
This isn't just about saving time; it's about precision. Pinpointing the exact boundary ensures radiation is blasted directly at the cancerous tissue while sparing the healthy parts, which can lead to better outcomes with fewer side effects.
This automated outlining not only takes minutes instead of hours but also introduces a level of consistency that's tough for even the most experienced human to replicate every single time. A proper AI requirements analysis is key to figuring out where automated segmentation can deliver the biggest impact for a clinical practice.
Triage: Finding the Needle in the Haystack, Fast
In a busy hospital, not all cases are created equal. Some are urgent, and others can wait. Triage models act as a digital gatekeeper, scanning every incoming study to flag the most critical findings that demand immediate attention.
Think of a radiologist in a swamped emergency department. A triage algorithm can run quietly in the background, analyzing every head CT as it comes in. If it spots signs of an intracranial hemorrhage, it instantly sends an alert and bumps that case to the very top of the worklist. That small shortcut can be the difference between life and death.
Systems like this are a game-changer for hospital efficiency and patient safety, which is a core goal of any well-designed AI Automation as a Service platform.
Prognostics: Peeking into the Future
Beyond just identifying what's happening now, prognostics uses machine learning to predict what might happen next. These sophisticated models analyze incredibly complex patterns in tissue or scans to forecast things like disease progression, patient survival, or how well someone might respond to a particular drug.
In pathology, for example, a prognostic model could analyze the cellular structure of a breast cancer biopsy. By picking up on patterns invisible to the human eye, it might predict a high likelihood of metastasis. That insight helps the oncologist decide if an aggressive treatment plan is necessary or if a more conservative approach is safe, paving the way for truly personalized medicine.
To tie it all together, these core functions form the basis of nearly every AI application in the diagnostic space.
Key Machine Learning Applications in Diagnostic Imaging
| ML Application | Core Function | Example in Radiology | Example in Pathology |
|---|---|---|---|
| Classification | Assigning a label to an image (e.g., normal/abnormal). | Identifying a lung nodule on a chest X-ray as either benign or suspicious for malignancy. | Classifying a prostate biopsy core as containing Gleason grade 3, 4, or 5 cancer cells. |
| Segmentation | Outlining a specific region or structure in an image. | Precisely delineating the boundaries of a glioblastoma on a brain MRI for treatment planning. | Automatically outlining regions of invasive carcinoma on a whole-slide image of a tumor. |
| Triage | Prioritizing urgent cases in a worklist. | Flagging a head CT scan with a suspected acute intracranial hemorrhage for immediate review. | Highlighting a slide with high-grade dysplasia that requires urgent pathologist confirmation. |
| Prognostics | Predicting future clinical outcomes from image data. | Analyzing tumor texture on a CT scan to predict a patient's response to immunotherapy. | Predicting the likelihood of cancer recurrence based on the spatial patterns of tumor cells. |
Understanding these distinct but often interconnected tasks is the first step in seeing how AI can be a practical, powerful partner in modern diagnostics.
Building the Business Case for AI in Your Practice
Bringing machine learning into your practice isn't just a tech upgrade—it's a serious business decision. And like any major investment, it requires a clear-eyed look at the return on investment (ROI). For most healthcare leaders, the question isn't "can AI do this?" It's "how will this really help my practice, my clinicians, and my patients?" The answer starts with building a business case that ties the technology directly to real, tangible results.
The use of machine learning in radiology and pathology is a direct response to some of the biggest headaches in healthcare today, like clinician burnout and those frustrating diagnostic delays. When you frame the investment as a solution to these core problems, it stops looking like an expense and starts looking like a vital tool for growth and better care.
Quantifying the Return on Investment
The ROI for AI in diagnostics isn't just one magic number; it’s a mix of direct financial gains and less obvious, but equally important, benefits. A solid business case needs to spell out both to give the full picture.
Direct Financial Benefits:
-
Increased Throughput: AI can speed up image analysis, which means a single radiologist or pathologist can get through more cases each day without sacrificing quality. This immediately boosts the practice's capacity to generate revenue.
-
Reduced Redundant Scans: When diagnostic confidence goes up, the need for follow-up scans and extra procedures often goes down. That cuts costs for everyone involved, from the provider to the patient.
-
Optimized Staffing: Automating the more repetitive, mundane tasks frees up your highly skilled clinicians to focus on what matters. This can reduce the pressure for overtime or hiring more staff just to keep up with the caseload.
Indirect Value and Risk Mitigation:
-
Enhanced Diagnostic Accuracy: Fewer mistakes lead to better patient outcomes, which is the ultimate goal. It also dramatically lowers the risk of facing expensive malpractice claims down the road.
-
Improved Clinician Retention: AI can take some of the tedious work off a clinician's plate, fighting burnout and creating a better work environment. In today's market, that’s a huge factor in keeping your best people.
-
Competitive Advantage: Let's be honest, practices that embrace this technology are seen as leaders. This helps attract not only top-tier medical talent but also patients who are looking for the most advanced care available.
Building a strong business case requires showcasing how technology solves real-world problems. For instance, it's essential to examine how AI helps healthcare practices save time and improve operational flow, as these are key drivers of financial health.
Developing a Strategic Advantage
Beyond the immediate numbers, AI offers a powerful long-term strategic edge. It’s about more than just buying software; it’s about rethinking how you work. This is where you can truly set your practice apart.
Instead of just relying on off-the-shelf solutions, you can create workflows perfectly suited to your team’s specific needs. Getting a clear roadmap together shifts the conversation from a simple cost-benefit talk to a serious discussion about future-proofing your practice. It’s about building a diagnostic service that’s more resilient, efficient, and ready for whatever comes next. With a well-crafted business case, you can get the buy-in you need to start that journey.
For a deeper look at how AI is being used across medicine, check out our insights on the https://www.ekipa.ai/industries/healthcare industry.
Your Pragmatic Roadmap for Clinical ML Implementation
Getting from a promising AI concept to a fully integrated clinical tool isn’t something you can rush. In my experience, successful adoption of machine learning in radiology and pathology happens in deliberate, well-planned stages. It's a journey that balances the excitement of innovation with the practical realities of a clinical setting.
This roadmap breaks that journey down, guiding you from a small, focused pilot to a full-scale deployment that genuinely makes a difference.
If you're looking for a higher-level view, this practical guide on how to implement AI in business offers a great framework that fits well with the clinical specifics we're discussing here. And make no mistake, the momentum is real. The U.S. market for AI in medical imaging is projected to hit USD 2.93 billion by 2030, growing at a blistering 33.24% CAGR from 2025. This isn't just hype; it's a direct response to physician shortages and crushing workloads. Radiology is leading the charge, with nearly 75% of the FDA's authorized AI/ML tools focused on medical imaging.
The timeline below gives you a bird's-eye view of how this phased approach works in practice.
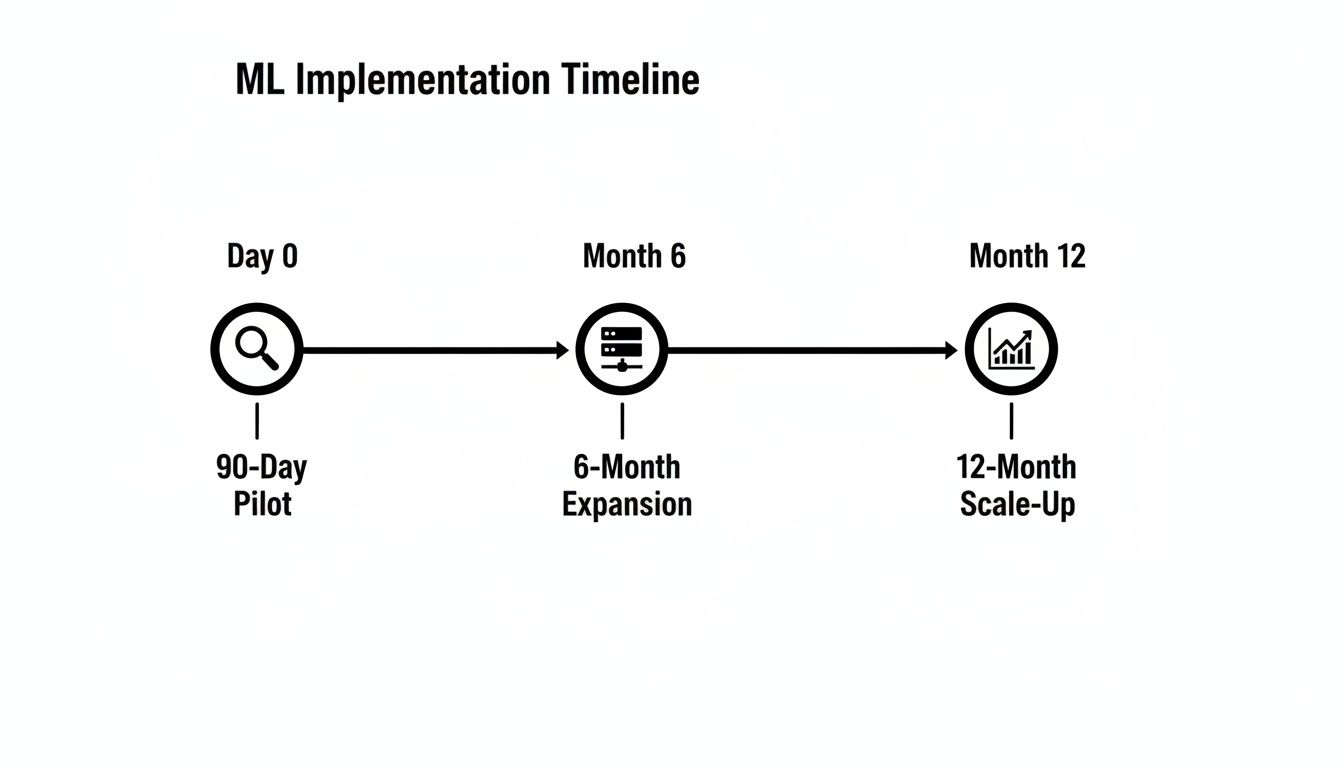
This kind of staged rollout is all about managing risk. It allows your team to learn, adapt, and build buy-in at every critical step.
The 90-Day Pilot Phase
Your first three months are all about proving the concept on a small scale. The goal here is simple: pick one high-impact use case and demonstrate a clear, undeniable win. You're not trying to revolutionize the whole department overnight; you're building momentum.
Key Actions:
-
Find the right pain point: Sit down with your clinicians. Is it the ever-growing backlog of routine mammograms? The tedious hours spent manually segmenting tumors for radiation oncology? Pinpoint a problem where an AI tool can deliver a fast, measurable improvement.
-
Choose a validated model: Don't reinvent the wheel. Partner with a vendor or select an off-the-shelf model that already has solid clinical validation and, ideally, regulatory clearance for your specific problem.
-
Define what success looks like: Set simple, unambiguous Key Performance Indicators (KPIs). For example, "reduce report turnaround time by 15%" or "achieve 95% accuracy in flagging suspicious lung nodules."
Think of the pilot as a controlled experiment. You're learning how the tool behaves with your data and your team in a safe environment, without disrupting the entire clinical workflow. It’s a low-risk way to gather the evidence you need to move forward.
The 6-Month Expansion Phase
With a successful pilot in your back pocket, the next six months are about going deeper with integration. This is where the technology stops being a standalone experiment and starts becoming a real part of your daily operations.
This stage demands a methodical approach. Integrating new tools into legacy systems is tricky, and a structured workflow is the only way to avoid technical headaches down the road. Our implementation support often focuses heavily on this phase to ensure the solution is robust and scalable.
Key Actions:
-
Connect to your core systems: This is a big one. Work with your IT department to plug the AI model directly into your Picture Archiving and Communication System (PACS) or Laboratory Information System (LIS). The goal is for the AI's output to appear seamlessly within the tools your radiologists and pathologists already use every day.
-
Validate on your own turf: Test the model's performance using data from your own patient population. This is critical for ensuring it works as expected in your specific real-world setting, not just in a lab.
-
Train a core user group: It's time to expand beyond the pilot team. Train a wider group of clinicians and, just as importantly, gather their honest feedback to iron out any workflow or usability issues.
The 12-Month Scale-Up Phase
Now you're ready for the final stage: expanding the solution across the entire department or even the health system. This is where you start to see the full return on your investment, making the tool a standard, indispensable part of care. But with scale comes the need for strong governance and monitoring.
Key Actions:
-
Map out the full deployment: Create a detailed rollout schedule. This should cover everything from training all staff who will interact with the tool to setting up clear technical support protocols.
-
Establish long-term KPIs: Your metrics should mature beyond the pilot. Start tracking long-term operational KPIs that measure sustained efficiency gains, diagnostic accuracy improvements, and the ultimate financial impact.
-
Form a governance committee: Assemble a multidisciplinary team to oversee the ongoing use of the AI. This group will be responsible for managing model updates, monitoring performance, and ensuring you always adhere to ethical and regulatory standards.
By following this pragmatic, three-phase roadmap, healthcare organizations can thoughtfully manage the use of machine learning in radiology and pathology, turning a powerful technology into a sustainable clinical asset that truly serves patients and clinicians alike.
Navigating the Ethical and Regulatory Landscape
Getting a machine learning model from the lab into a live clinical setting isn't just about the tech. It’s a serious undertaking that involves navigating a maze of ethical questions and stringent regulations. Overlooking this part of the journey can completely sink an otherwise brilliant project.
This is where the rubber meets the road—where algorithms and accountability intersect. It's not enough for a model to be accurate. It has to be fair, transparent, and secure. Successfully managing this requires a firm grasp of the clinical and legal frameworks that protect patients, something we build into every AI strategy we consult on.
Demystifying Regulatory Approvals
Before any AI tool touches a patient's case in the US, it needs a green light from the FDA. In Europe, it needs a CE mark. Think of these as a non-negotiable seal of approval, a guarantee that the tool is both safe and effective for clinical use.
The approval process is anything but a rubber stamp. It's a demanding, data-heavy journey that requires extensive clinical validation. You have to prove the model performs as promised by testing it against human experts and established medical standards, using data from a wide variety of patient groups. This isn't just about showing it works; it's about proving it won't introduce new risks into the diagnostic process.
The Challenge of Algorithmic Bias and Explainability
Two of the toughest ethical knots to untie in medical AI are bias and the infamous "black box" problem.
-
Algorithmic Bias: An AI model is a mirror of its training data. If that data mostly comes from one demographic, the model will inevitably struggle with underrepresented groups. This isn't just a technical flaw; it can create real-world health disparities. Fighting bias is an absolute ethical imperative.
-
The Black Box Problem: Many of the most powerful deep learning models are incredibly complex. They give you an answer, but they can't always tell you how they got there. A radiologist or pathologist can't just blindly trust an output; to take responsibility for a diagnosis, they need to understand the model's logic.
Tackling these issues head-on is the only way to build trust with clinicians and patients. An AI tool that’s biased or opaque isn’t just a bad tool—it’s an irresponsible one. This is exactly where our expert team steps in, guiding organizations to build solutions that are both equitable and transparent.
Data Governance and Patient Privacy
Protecting patient data is the absolute top priority. Machine learning in diagnostics deals with huge volumes of highly sensitive information, so rock-solid data governance is essential. That means strict compliance with regulations like HIPAA, which sets the legal standard for protecting patient health information (PHI).
One of the most exciting solutions to this challenge is federated learning. This clever approach trains AI models across different hospitals or clinics without the sensitive data ever leaving the premises. It's a game-changer, allowing us to build powerful, diverse models while keeping patient privacy locked down. For those looking for more advanced solutions, custom healthcare software development can ensure these privacy features are built-in from the ground up.
This isn't just a local issue. The global push for this technology is undeniable. In China, for example, where radiologists are buried under massive caseloads, AI is being adopted quickly to keep up. It's a perfect illustration of the worldwide demand for efficient tools that don't compromise on privacy. You can discover more about these global AI radiology trends from Grand View Research.
By thoughtfully addressing these regulatory, ethical, and data challenges, healthcare providers can bring powerful AI solutions into their daily work, ensuring that every new innovation truly serves patients safely and effectively.
The Future of Diagnostics: Human-AI Collaboration
As we look ahead, one thing becomes crystal clear: the use of machine learning in radiology and pathology is about partnership, not replacement. The goal isn’t to build an AI that makes diagnoses in a vacuum. It’s to forge a powerful collaboration where human expertise is magnified by the analytical power of machine learning.
This model is sometimes called the "centaur radiologist" or "centaur pathologist." Think of the mythical centaur—a blend of human intelligence and a horse's strength. In the same way, this approach combines a clinician's years of medical knowledge with an AI's phenomenal speed in processing data. The AI does the heavy lifting of pattern detection, while the clinician provides the essential context, nuance, and final diagnostic judgment.
This setup frees up medical experts to work at the top of their game. They can focus their attention on the most complex cases and critical decisions instead of getting mired in repetitive analytical work.
The Rise of Multimodal AI
The next major step is multimodal AI, a technology that promises a truly complete picture of patient health. Right now, most AI models are trained on a single type of data, like a CT scan or a pathology slide. Multimodal AI tears down those walls.
Imagine a system that does more than just analyze a chest X-ray. It simultaneously considers:
-
Notes from the patient’s electronic health record (EHR).
-
Genomic data highlighting specific genetic markers.
-
Recent lab results from blood work.
By weaving these different threads together, the model can spot connections that would be almost impossible for a human to see. This comprehensive view helps shift medicine from being reactive—treating diseases after they show up—to being proactive and predictive. It's the groundwork for truly personalized medicine.
From Reactive to Proactive Medicine
This isn't just a technical upgrade; it's a fundamental change in how we approach healthcare. Instead of simply finding a tumor, future AI could predict its likely growth pattern, recommend the best chemotherapy based on its genetic makeup, and flag patients at high risk for recurrence long before physical symptoms appear.
The ultimate goal is to catch disease at its earliest, most treatable stage—or even before it starts. This proactive stance is where machine learning delivers its greatest value, creating a healthcare system that is more preventative, personalized, and effective.
Getting to this future requires a clear vision and a deliberate plan. It starts by taking stock of where your organization is today and finding the best opportunities to bring in AI. Developing internal tooling and looking at proven real-world use cases are vital first steps.
To start charting your own course, a Custom AI Strategy report can offer the clarity you need to make these future possibilities a clinical reality. Connect with our expert team to learn how you can begin building the future of diagnostics today.
Frequently Asked Questions
When it comes to bringing machine learning into radiology and pathology, it's natural to have questions. Getting a handle on the real-world impact is the first step toward making smart decisions. Here are some of the most common questions we hear from healthcare leaders looking at these powerful AI solutions.
Will AI and Machine Learning Replace Radiologists and Pathologists?
The short answer is no. The consensus in the field is that AI is here to assist, not replace, these highly trained experts. Think of it this way: machine learning is brilliant at the tireless, repetitive work—like flagging thousands of potential nodules or meticulously counting cells—that can bog down a specialist.
What AI can't do is replicate the nuanced clinical judgment, complex reasoning, and deep contextual understanding that come from years of human experience. The future is a partnership. The clinician remains the final authority, the "human-in-the-loop," who validates the AI's findings. This frees them up to focus on the most complex cases, talk with patients, and guide treatment strategy, ultimately making the entire diagnostic process sharper and more efficient.
What Are the Biggest Barriers to Adopting ML in a Clinical Setting?
Getting AI into a live clinical environment usually comes down to three major hurdles: integration, regulation, and data.
First, there's the technical challenge of weaving new AI tools for business into the fabric of your existing IT infrastructure. Getting them to talk seamlessly with legacy PACS and LIS systems takes real planning. Second, the regulatory path is steep. Gaining clearance from bodies like the FDA or getting a CE mark requires rock-solid clinical validation to prove an algorithm is both safe and effective.
Finally, data is the elephant in the room. You need massive amounts of high-quality, diverse data to train and test these models, and that's all tangled up in patient privacy laws like HIPAA. A clear plan, a deep understanding of compliance, and expert guidance from AI strategy consulting are essential for navigating these waters. As we explored in our AI adoption guide, taking it one step at a time is the best way to manage the risk.
How Can a Small Clinic or Hospital Get Started with Machine Learning?
Start small, and aim for a clear, tangible win. You don't need to reinvent your entire department overnight. The best approach is to pick a single, high-impact problem and launch a focused pilot project.
For example, you could start with an AI tool that helps triage chest X-rays, automatically flagging the most critical cases for immediate review. Or you might use an algorithm to automate a routine but time-consuming measurement.
Cloud-based AI platforms have made this much more accessible, removing the need for a huge upfront investment in hardware. A well-defined pilot project proves the value quickly, helps get clinicians on board, and teaches you crucial lessons about integration and workflow before you commit to a larger rollout. A Custom AI Strategy report can pinpoint the perfect place to start, based on your team's unique needs and resources. To get started on your own journey, feel free to connect with our expert team.



